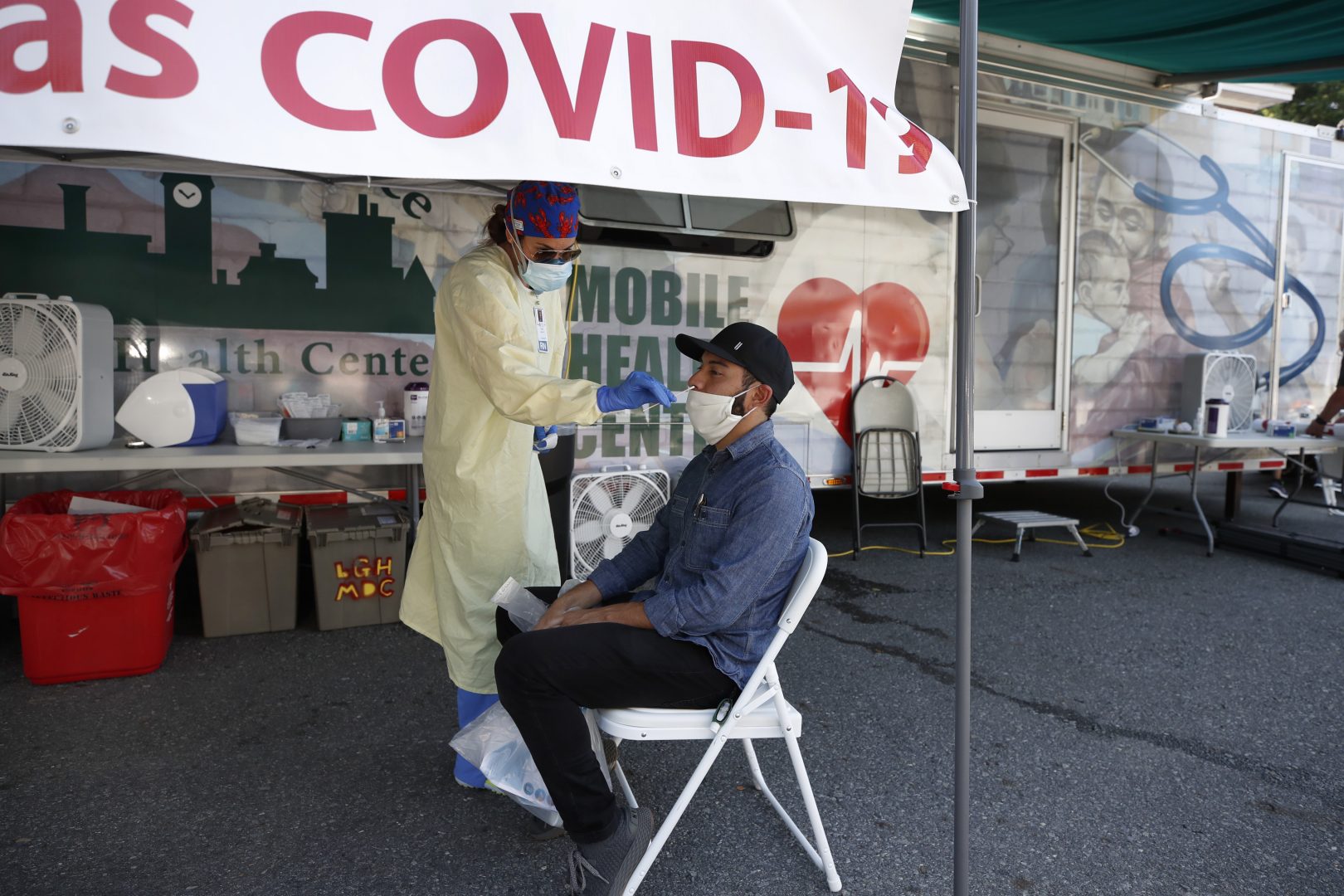
Nurse Tanya Markos administers a coronavirus test on patient Ricardo Sojuel at a mobile COVID-19 testing unit, Thursday, July 2, 2020, in Lawrence, Mass.
Elise Amendola / AP Photo

Nurse Tanya Markos administers a coronavirus test on patient Ricardo Sojuel at a mobile COVID-19 testing unit, Thursday, July 2, 2020, in Lawrence, Mass.
Elise Amendola / AP Photo

Elise Amendola / AP Photo
Nurse Tanya Markos administers a coronavirus test on patient Ricardo Sojuel at a mobile COVID-19 testing unit, Thursday, July 2, 2020, in Lawrence, Mass.
(Washington) — Throughout the U.S., hospitals and health care workers are tracking the skyrocketing number of new coronavirus cases in their communities and bracing for a flood of patients to come in the wake of those infections. Already, seriously ill COVID-19 patients are starting to fill up hospital beds at unsustainable rates.
U.S. hospitalizations overall have nearly doubled since late September. As of Monday more than 56,000 COVID-19 patients were hospitalized around the country, approaching the highs of the midsummer and spring surges.
Loading…
“We have legitimate reason to be very, very concerned about our health system at a national level,” says Lauren Sauer, an assistant professor of emergency medicine at Johns Hopkins University who studies hospital surge capacity.
The spring and summer waves of COVID-19 hospitalizations were concentrated largely in a handful of cities in the Northeast and parts of the South.
With the virus now surging across the country, experts warn the impact of this next wave of hospitalizations will be even more devastating and protracted.
“I fear that we’re going to have multiple epicenters,” says Dr. Mahshid Abir, an emergency physician at the University of Michigan and researcher at the RAND Corporation, who has developed a model that helps hospitals manage surge capacity.
If that happens, Abir warns there won’t be flexibility to shuffle around resources to the places in need because everywhere will be overwhelmed.
Loading…
The impact varies state by state, with certain areas showing much more rapid increases in hospitalizations. As of Monday, hospitalizations are now rising in 47 states, according to data collected by The Covid Tracking Project and 22 states are seeing their highest numbers of COVID-19 hospitalizations since the pandemic began.
Where are hospitals at risk of maxing out?
With the numbers growing nearly everywhere, the key question for hospital leaders and policy makers is, when is a community on the brink of having more patients than it can handle?
In parts of the Midwest the West, hospitals are already brushing up against their capacity to deliver care. Some are struggling to find room for patients, even in largeurban hospitals that have more beds.
But the surge in hospitalizations is not evenly spread — and hospitals’ capacity for weathering case surges varies greatly.
One way to gauge the growing stress on a health care system is by tracking the share of hospital beds occupied by COVID-19 patients.
The federal department of Health and Human Services tracks and publishes this data at the state (but not the local) level. Several experts NPR spoke to say that, though imperfect, this is one of the best metrics communities have to work with.
Loading…
Though there’s not a fixed threshold that applies to all hospitals, generally speaking, once COVID-19 hospitalizations exceed 10% of all available beds, that signals an increasing risk that the health care system could soon be overwhelmed, explains Sauer.
“We start to pay attention above 5%,” says Sauer. “Above that, 10% is where we think, ‘Perhaps we have to start enacting surge strategies and crisis standards of care in some places.’”
Crisis standards of care is a broad term for how to prioritize medical treatment when resources are scarce. In the most extreme cases, that can lead to rationing of care based on a patient’s chance of survival.
The latest data from HHS shows that 18 states — mostly in the Midwest — COVID-19 hospitalizations have already climbed above 10%.
Six states are over 15%, including North Dakota and South Dakota, which are now over 20%.
Hospital capacity is flexible … until it’s not
The percent of hospital beds taken up by COVID-19 patients does not tell a complete story about hospital capacity, says Sauer, but it’s a starting point.
Hospital capacity is not so much a static number, but an ever-shifting balance of resources. “It’s space, staff and stuff, and you need all three, and if you don’t have one, it doesn’t matter if you have the other two,” says Abir.
The level of COVID-19 hospitalizations that would be a crisis in one place, might not be in another. Still a growing share of beds occupied by COVID patients can be a strong signal that the health care system is headed for trouble.
COVID-19 patients can be more labor intensive because health care workers have to follow intricate protocols around personal protective equipment and infection control. And some of the patients take up ICU space.
“When the numbers go up like that, particularly for critical care, that strains the system pretty significantly,” says Dr. Abir. “This is a scarce resource. Critical care nurses are scarce. Ventilators are scarce. Respiratory therapists are scarce.”
In Utah, where the share of hospitalized COVID patients is about 8%, state health officials have already warned hospitals may soon be forced to ration care because of limited ICU space.
There is no “magic number” to indicate when a health care system may be overwhelmed, says Eugene Litvak, who is CEO of the Institute for Healthcare Optimization and helps advise hospitals on how to manage their capacity. But hospitals must be alert to rapid increases in patient load.
“Even a 10% increase can be quite dangerous,” says Litvak. “If you are a hospital that’s half empty, you can tolerate it.” But Litvak says generally U.S. hospitals run close to capacity, with above 90% of beds already full, especially toward the end of the week.
“Imagine that 10% of extremely sick patients on top of that,” he says. “What are your options? You can not admit ambulances and patients with non-COVID medical needs, or you have to cancel your elective surgeries.”
In the spring, some states ordered that most elective surgeries come to a halt so that hospitals had room for COVID-19 patients, but Litvak says this leads to all kinds of collateral damage, because patients don’t get the care they need and hospitals lose money and lay off staff.
State data may miss local hot spots
Statewide COVID-19 hospitalization metrics mask huge variations within a state. Certain health care systems or metro areas may be in crisis.
“It’s very valuable information, but a state average can be misleading,” says Ali Mokdad with the Institute of Health Metrics and Evaluation at the University of Washington, which projects that many states will face big problems with hospital capacity this winter. “It doesn’t tell you where in the states it’s happening.”
Big urban centers may be much better equipped to absorb a rush of patients than smaller towns.
In New York City, Mount Sinai Health System was able to more than double its bed capacity during the spring surge. Other communities don’t have the ability to ramp up capacity so quickly.
“Especially the states that don’t have major cities with major hospitals, you see a lot of stress on them,” Mokdad says.
But it’s hard for researchers and health leaders to get a clear picture of what’s happening regionally without good data, he adds. NPR has reported that the federal government does not share this local data, although it does collect it daily.
Some states publish their own hospital data sets. Texas, which shares the data in detail, provides a striking example. Statewide, COVID-19 hospitalizations have reached about 11%. Meanwhile, El Paso is at over 40%, which has pushed the health care system to the brink.
Loading…
Ultimately, it’s difficult to know the true capacity for a region because many hospitals still don’t coordinate well, says Dr. Christina Cutter, an emergency physician at the University of Michigan who collaborated on the RAND model with Dr. Abir.
“It’s really hard to make sure you’re leveraging all the resources and that one hospital is not overburdened compared to another hospital and that may have unintended loss of life as a consequence,” Cutter says.
Dire consequences of overfilled hospitals
During the height of Arizona’s summer surge, COVID-19 patients filled nearly half of all beds in the state.
“When 50% of our hospital is doing COVID, it means the hospital is overloaded. It means that other services in that hospital are being delayed,” says Mokdad. “The hospital becomes a nightmare.”
Health care workers are pushed to their limits and are required to treat more patients at the same time. Hospitals can construct makeshift field hospitals to add to their capacity like Wisconsin, but those can be logistically challenging and still require health care workers to staff the beds.
In Wisconsin, COVID-19 patients account for 17% of all hospitalizations, and many hospitals are warning that they are at or near capacity.
The Marshfield Clinic Health System, which runs nine hospitals in primarily rural parts of the state, is expecting its share of COVID-19 patients to double, if not more, by the end of the month.
“That will push us well beyond our staffing levels,” says Dr William Melms, chief medical officer at Marshfield. “We can always make more space, but creating the manpower to take care of our patients is the dilemma.”
During earlier surges, many hospitals relied on bringing in hundreds or even thousands of out-of-state health care workers for backup, but Melms says that is not happening this time.
“We are on an island out here,” he says.
An increase in COVID-19 hospitalizations statewide is also associated with higher mortality, according to a recent study that analyzed the relationship between COVID-19 hospitalizations and deaths.
“It’s an indicator that you’re going to have more deaths from COVID as you see the numbers inch up in the hospital,” says Pinar Karaca-Mandic, professor and academic director of the Medical Industry Leadership Institute at the University of Minnesota.
Specifically, Karaca-Mandic’s research found that a 1% increase of COVID patients in a state’s ICU beds will lead to about 2.8 additional deaths in the next seven days.
She says a statewide level of 20% COVID hospitalizations may not look all that alarming, but that number doesn’t capture the constraints on the health care system in adding more ICU beds.
“That’s not very flexible,” she says. “It requires a lot of planning. It requires a lot of investments. So the more you fill up the ICU, the impact is going to be larger.”
The days of journalism’s one-way street of simply producing stories for the public have long been over. Now, it’s time to find better ways to interact with you and ensure we meet your high standards of what a credible media organization should be.